Diabetic Slippers Womens for Plantar Fasciitis EPTODT160
Product code : EPT-ODT-160
Colours
|
Womens slipper sizes
|
TELEFONDA SİPARİŞ VER
+90 212 671 20 21
Tıklayın, telefonunuzu bırakın. Sizi arayalım.
Diabetic Slippers Womens for Plantar Fasciitis
► Best slippers for plantar fasciitis
► Heel cushion support with special silicone
► First quality soft genuine leather
► Best quality orthopedic insole
► Women’s diabetic slippers for plantar fasciitis size: 36-37-38-39-40-41
► 4 Seasonal models.
► Antibacterial and don’t sweat.
► Suitable for women’s foot anatomy.
► Best comfortable slippers for diabetic feet
► Increase the quality of your life and walk
► PU outsole
► Anti-slip outsole design
► Colours: Black, beige, brown
► Model code: EPT-ODT-160
► Closed toe slippers
► Made in Türkiye
► Brand: Ladyfalcon
► Full protection for injury
► Wide toe area
► No stitches or stitches that are used very little
► Memory sponge
► The height of the toe part of the polyurethane sole is 1.50 cm and the heel height is 3.50 cm.
Benefits of Using Diabetic Slippers for Plantar Fasciitis ;
► Diabetic slippers provide full protection for injury.
► Minimizes the negative effects of diabetes on the feet.
► Provides protection for infection and ulcers.
► Comfortable finger zone.
► Reduce your heel pain thanks to the silicone-supported heel area
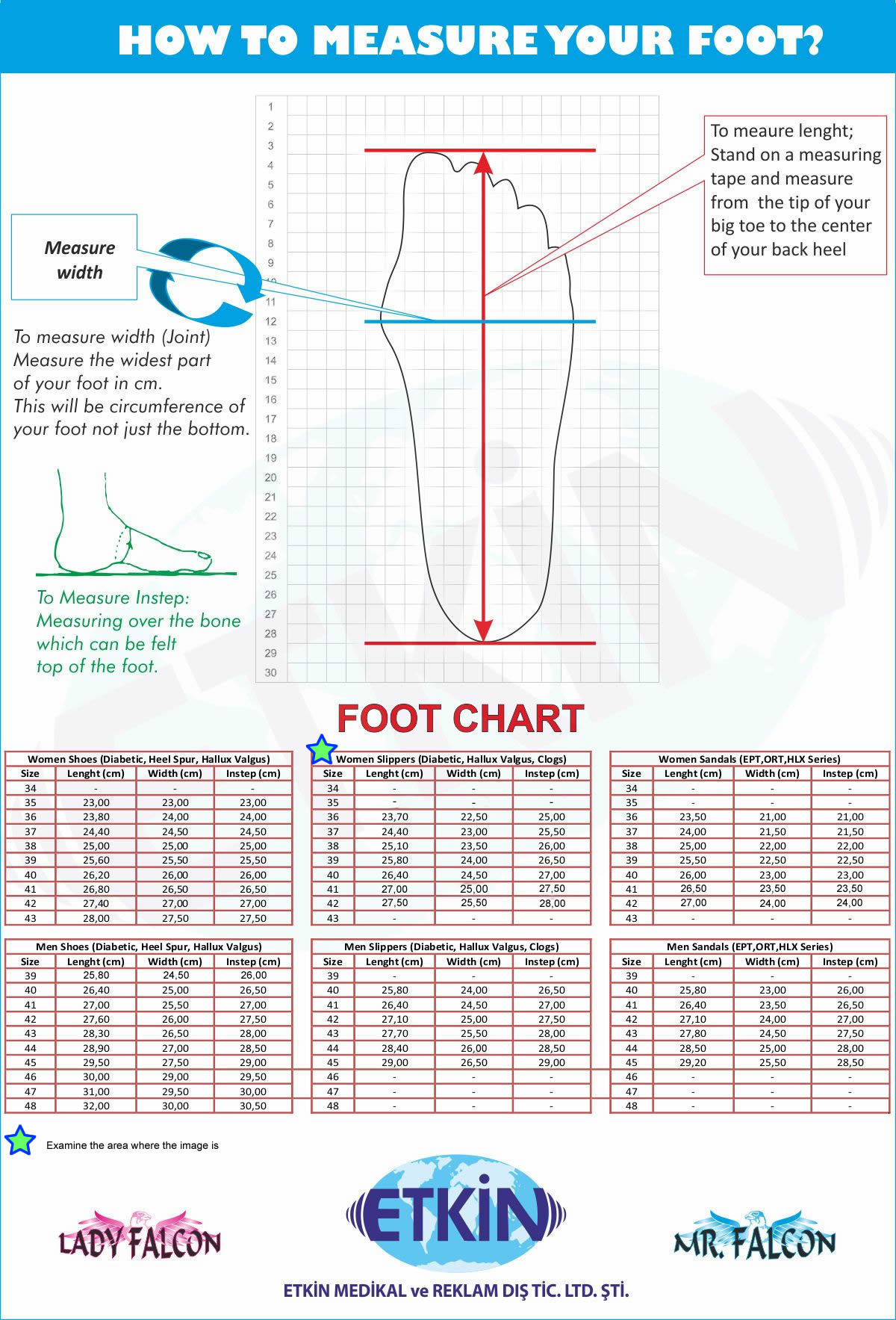
How To Measure Your Foot?
* Look at diabetic slippers for plantar fasciitis field in the table below.
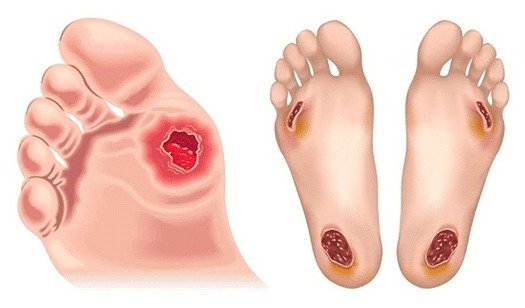
What is the importance of using diabetic slippers for diabetic patients?
Using diabetic slippers is essential for diabetic patients due to the following reasons:
» Foot Protection: Diabetic slippers are designed with soft and non-abrasive materials to protect the feet from injuries, reducing the risk of cuts, bruises, and blisters, which can be more concerning for individuals with diabetes.
» Pressure Redistribution: These slippers offer extra cushioning and support, distributing pressure evenly across the feet, minimizing the formation of pressure points and potential foot complications.
» Diabetic Neuropathy: Diabetic patients often experience neuropathy, a condition that affects nerve sensitivity. Diabetic slippers with soft interiors prevent irritation and reduce the risk of foot ulcers.
» Breathability: Diabetic slippers are typically made from breathable materials, promoting airflow and reducing moisture accumulation, which helps prevent fungal infections.
» Customized Fit: They come in various sizes and widths, allowing for a personalized fit that accommodates any foot deformities or swelling that may occur in diabetic patients.
» Comfort and Relief: Diabetic slippers offer comfort and relief from foot pain and discomfort, making them ideal for individuals with sensitive and tender feet.
» Wound Healing Support: For those with existing foot ulcers or wounds, diabetic slippers provide a gentle and protective environment, aiding in the healing process.
» Fall Prevention: Diabetic slippers with non-slip soles help prevent accidental slips and falls, ensuring safety and stability while walking.
» Diabetic Foot Care: Using diabetic slippers as part of a comprehensive foot care routine helps maintain better foot health and manage diabetic conditions effectively.
» Mobility and Independence: The comfortable design of diabetic slippers enables individuals to move freely and maintain an active lifestyle while taking care of their feet.
It is crucial for individuals with diabetes to consult healthcare professionals or podiatrists to choose the most suitable diabetic slippers based on their specific needs and foot condition. Regular foot care, including the use of appropriate footwear like diabetic slippers, is essential in preventing complications and promoting overall foot health.
What is Diabetes?
Diabetes is a disease that occurs when your blood glucose, also called blood sugar, is too high. Blood glucose is your main source of energy and comes from the food you eat. Insulin, a hormone made by the pancreas, helps glucose from food get into your cells to be used for energy. Sometimes your body doesn’t make enough—or any—insulin or doesn’t use insulin well. Glucose then stays in your blood and doesn’t reach your cells.
Over time, having too much glucose in your blood can cause health problems. Although diabetes has no cure, you can take steps to manage your diabetes and stay healthy.
Diabetes is a chronic medical condition that affects how your body processes glucose (sugar) from the food you eat. The hormone insulin, produced by the pancreas, helps regulate the amount of glucose in your blood. In people with diabetes, there are issues with insulin production, action, or both, leading to elevated blood sugar levels.
There are three main types of diabetes:
» Type 1 diabetes: It occurs when the immune system mistakenly attacks and destroys the insulin-producing cells in the pancreas. As a result, the body produces little to no insulin. Type 1 diabetes is usually diagnosed in children and young adults and requires lifelong insulin therapy.
» Type 2 diabetes: This is the most common form of diabetes, characterized by insulin resistance, where the body's cells do not respond properly to insulin. Initially, the pancreas compensates by producing more insulin, but over time, it may not produce enough to control blood sugar effectively. Type 2 diabetes is often associated with lifestyle factors such as obesity, sedentary lifestyle, and poor dietary habits. It can sometimes be managed with lifestyle changes, medication, and, in some cases, insulin therapy.
» Gestational diabetes: This type of diabetes occurs during pregnancy when hormonal changes can lead to insulin resistance. It usually resolves after childbirth, but women who experience gestational diabetes are at a higher risk of developing type 2 diabetes later in life.
What are the diabetes treatment options?
Treatment options for diabetes depend on the type and severity of the condition. The primary goals of diabetes management are to control blood sugar levels, prevent complications, and improve quality of life. Here are some common treatment options:
» Lifestyle modifications: For prediabetes and type 2 diabetes, lifestyle changes play a crucial role in managing the condition. These include adopting a balanced diet, engaging in regular physical activity, losing weight if overweight or obese, and quitting smoking if applicable.
» Oral medications: People with type 2 diabetes may be prescribed various oral medications that help improve insulin sensitivity, reduce glucose production in the liver, or stimulate insulin release.
» Insulin therapy: People with type 1 diabetes and some with type 2 diabetes may require insulin injections to regulate blood sugar levels. Insulin can be administered using syringes, insulin pens, or insulin pumps.
» Glucose monitoring: Regular blood glucose monitoring is essential for people with diabetes to keep track of their sugar levels and adjust their treatment plan accordingly.
» Continuous Glucose Monitoring (CGM): CGM devices can provide real-time information about blood sugar levels, helping patients and healthcare providers make more informed treatment decisions.
Bariatric surgery: In some cases of severe obesity-related type 2 diabetes, bariatric surgery may be considered as an option to improve blood sugar control and promote weight loss.
It's important to note that diabetes management should be personalized to each individual's needs, and regular follow-up with healthcare professionals is essential to adjust treatment plans as needed. Additionally, diabetes self-management education and support programs can help individuals learn how to manage their condition effectively.
Who Is At Risk For Diabetes?
» Obesity or being overweight. Research shows this is a top reason for type 2 diabetes. Because of the rise in obesity among U.S. children, this type is affecting more teenagers.
» Impaired glucose tolerance. Prediabetes is a milder form of this condition. It can be diagnosed with a simple blood test. If you have it, there’s a strong chance you’ll get type 2 diabetes.
» Insulin resistance. Type 2 diabetes often starts with cells that are resistant to insulin. That means your pancreas has to work extra hard to make enough insulin to meet your body’s needs.
» Ethnic background. Diabetes happens more often in Hispanic/Latino Americans, African-Americans, Native Americans, Asian-Americans, Pacific Islanders, and Alaska natives.
» Gestational diabetes. If you had diabetes while you were pregnant, you had gestational diabetes. This raises your chances of getting type 2 diabetes later in life.
» Sedentary lifestyle. You exercise less than three times a week.
» Family history. You have a parent or sibling who has diabetes.
» Polycystic ovary syndrome. Women with polycystic ovary syndrome (PCOS) have a higher risk.
» Age. If you’re over 45 and overweight or if you have symptoms of diabetes, talk to your doctor about a simple screening test.
What is Heel Spurs?
A heel spur is a bony growth that develops on the underside of the heel bone, also known as the calcaneus. It is often associated with a condition called plantar fasciitis, but it can also occur independently. Here's more information about heel spurs:
» Formation: Heel spurs typically develop over a period of time due to repeated strain or stress on the foot's ligaments and muscles. One common cause is the excessive pulling of the plantar fascia, a thick band of tissue that runs along the bottom of the foot, connecting the heel to the front of the foot. This pulling can lead to the development of a bony protrusion at the point where the plantar fascia attaches to the heel bone.
» Symptoms: Heel spurs themselves often don't cause noticeable pain. The pain and discomfort associated with heel spurs usually stem from the underlying condition, such as plantar fasciitis. However, if the spur becomes large or rubs against other structures in the foot, it can cause localized pain and discomfort.
» Relationship with Plantar Fasciitis: While heel spurs are often associated with plantar fasciitis, it's essential to note that the presence of a heel spur doesn't necessarily mean you have plantar fasciitis. Many people have heel spurs without experiencing significant pain. Plantar fasciitis is primarily caused by inflammation of the plantar fascia, and the symptoms are related to this inflammation rather than the spur itself.
» Diagnosis and Treatment: Heel spurs are typically diagnosed through imaging tests, such as X-rays. If the spur is causing significant pain or discomfort, treatment options may include rest, ice, anti-inflammatory medications, physical therapy, custom orthotic devices, and appropriate footwear with arch support. In some cases, corticosteroid injections or other medical interventions might be considered. Surgical removal of the spur is rare and usually only considered if conservative treatments have been ineffective and the pain is severe.
It's crucial to consult with a healthcare provider, particularly a podiatrist or orthopedic specialist, if you suspect you have a heel spur or are experiencing persistent heel pain. They can properly diagnose the underlying cause and recommend the most appropriate treatment based on your specific situation.
Check out the products / categories below that we think might be of interest to you
Can I shop safely on your site?
All purchases you make through https://www.medicalfootwear.net use the latest technologies and the best service provider for your safety.
Once you enter your credit card number under SSL security, you can be sure that no one will have access to this information. No one can view or access your information except you. The information about your number is encrypted and sent to your bank if you enter your credit card number. Your information can not be accessed by third parties, including https://www.medicalfootwear.net in this sense. Your card information is only known and protected by you and your bank.
Product price : 189.00 USD
When are orders shipped?
Products are generally shipped within 1-5 business days.
When will my order be delivered?
Products shipped are usually delivered to your address within 3-7 business days.
We ship with Fedex, DHL, UPS adn TNT, which are the leading cargo companies of express courier transportation. If you have a different request, please contact our company.
Where can I track my order?
You can track your order in the “my orders” section on our website. In addition, you can track the shipment directly by clicking on the link that is sent to your email address.
I cannot access the tracking information for my order. What am I supposed to do?
You need to contact us directly or through our support department if you encounter such a problem.
Which regions do you ship to?
You can shop online from anywhere in the world.
Safe Shopping
Free Shipping
Shipping Within 1-5 Days
Best Quality Products